Modern Medicine and Capitalism may be compatible with one another, but both are at odds with the real essence of the word healthcare.
Modern medicine treats the human body as a mechanical entity where all of its parts are replaceable in kind, or its near mechanical substitute.
 Much like one replaces the tires of his car once in a while to maintain a good grip on the road and avoid accidents, the surgeon cuts the severed limbs of a soldier who just survived from an IED explosion, and replace them with prosthetics.
Much like one replaces the tires of his car once in a while to maintain a good grip on the road and avoid accidents, the surgeon cuts the severed limbs of a soldier who just survived from an IED explosion, and replace them with prosthetics.
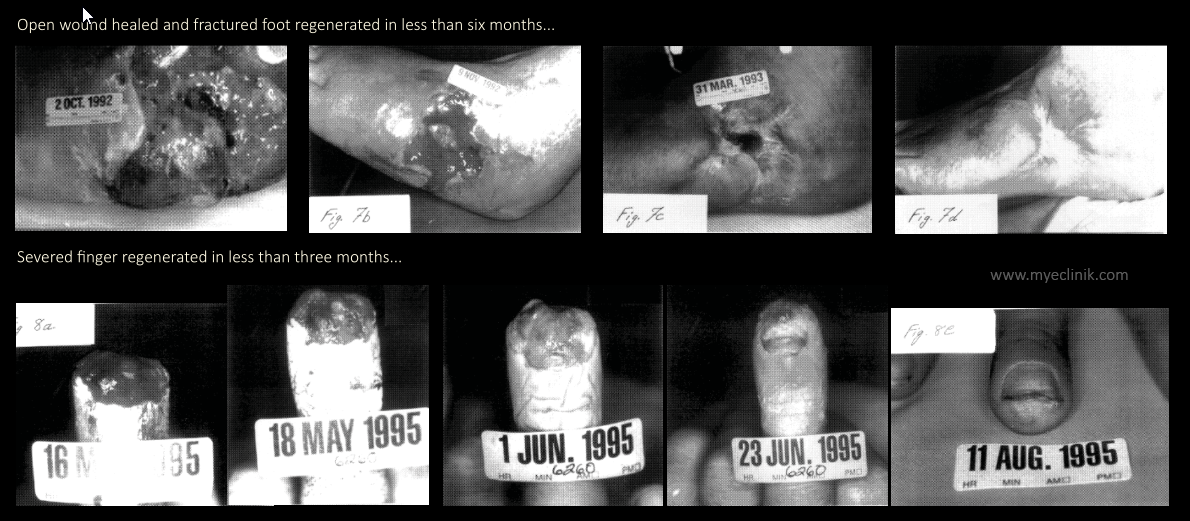
People stand in awe of the variety of smart bionic limbs out there, until they became aware that one can regrow his entire limb with a just a little help of simple medical science known as bone regeneration through electrostimulation.
“The sheaths surrounding the nerves are not merely insulation as described in established biology but are ‘real wire’ that reach into each area of the body to create a normal electrical environment around each cell, or a stimulatory one when healing growth is needed.” Dr. Robert O. Becker
The same science could be utilized for other organs, too.
But there is better profit in manufacturing, marketing and installation of industrially manufactured body parts. In fact, there is an entire collection of industries that could be wiped out if all one needs to do is switch on a little gadget that can deliver a millivolt of stimulant to the sheath of the bone needing regrowth.
What keeps us from the most practical solution to surgery is capitalism and the people who introduced and control the whole system.
In a saner society, we could bring down the cost of healthcare and raise its quality at the same time.
Otherwise, we have to endure these…
Filthy surgical instruments: The hidden threat in America’s operating rooms
By Joe Eaton 7:00 am, February 22, 2012 Updated: 12:19 pm, May 19, 2014
It seemed simple enough at the time. In 2009, John Harrison, a 63–year-old oil industry sales manager in Mission, Texas, had surgery to repair the rotator cuff in his right shoulder, a routine procedure that usually requires at most a single night’s stay in the hospital, followed by physical therapy. For Harrison, however, there was nothing routine about the ordeal that ensued.
In the weeks following the surgery, his scar turned bright red, hot to the touch, and oozed thick fluid that looked “like butter squeezed from a bag.” Alarmed, Harrison’s wife, Laura, called The Methodist Hospital in Houston, where the surgery was performed. The doctor urged Harrison to immediately make the seven-hour drive back to Houston for an emergency checkup.
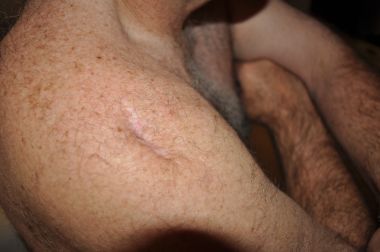
That night, surgeons opened up Harrison’s shoulder and found that infection had eaten away part of his shoulder bone and rotator cuff. Screws and metal hardware surgeons placed in his shoulder had pulled loose. Sutures had come undone. Surgeons cleaned out Harrison’s shoulder, installed two drains and gave him antibiotics to battle the infection.
When Harrison awoke from that surgery, he imagined his nightmare was over. But in reality, it had just begun. Since then, what began as a simple operation has turned into a lengthy struggle that left him for months at a time dependent on hired nurses, unable to dress himself, take a shower, or work, and afraid for his life.
“I’m a pretty tough guy, being in the oil patch,” said Harrison, a soft-spoken man who tends to understate the severity of his ordeal. But the pain “felt like someone hit your shoulder with a baseball bat with a razor blade attached to it.”
Harrison at first blamed himself, thinking he had not taken proper care of his surgical wound. The truth was much worse: Harrison was one of at least seven joint surgery patients at Methodist who acquired dangerous infections during a two-week period. The outbreak led Methodist to close operating rooms and cancel knee and shoulder surgeries while hospital and Centers for Disease Control and Prevention (CDC) investigators searched for the cause.
They found two likely sources in unlikely, yet terrifying, spots — deep inside a hand-held power tool called an arthroscopic shaver, which surgeons use to shave away bone and tissue during surgery, and inside a long narrow metal tube called an inflow/outflow cannula, which is used to irrigate and suction the surgical site.
Flawed and Poor Quality Surgical Instruments Place Patients at Risk
December 31, 2016
https://youtu.be/Glm5RxOnmkc
By Dr. Mercola
The BBC documentary, “Surgery’s Dirty Secrets,” which originally aired in 2011, investigates the sources of surgical tools, and highlights flaws in British safety regulations.
If you’re like most, you probably assume that surgical instruments are made to the very highest, exacting standards. The reality of where and how these tools are made is downright shocking.
According to BBC reporter Samantha Poling, who spent a year investigating this topic, there are significant problems in the industry — problems that can, and have, caused severe illness and death.
An estimated 30 million operations are carried out in British hospitals each year. In order to perform, surgeons need the right tools for the job, and these tools must be made to exact specifications and be of the highest quality.
Poorly made or non-functioning surgical tools can mean the difference between a successful surgery and the loss of a limb or organ, or death of the patient.
For example, for each fraction of a second a surgical assistant is struggling with a poorly functioning arterial clamp, the patient is losing blood, compromising the success of the surgery.
Lethal Infections Spread by Surgical Tools
In 2009, Dorothy Brown underwent heart surgery at Nottingham City Hospital. While the operation was a success, she contracted an antibiotic-resistant infection that nearly claimed her life. Ten other patients operated on by Brown’s surgeon around the same time contracted the same lethal infection.
Five of them subsequently died. In the U.S., the Food and Drug Administration (FDA) reports at least 1,000 incidences where poor quality surgical instruments have caused harm each year.
A confidential report obtained by Poling reveals the two most likely causes of the mass infection at Nottingham City Hospital were either air born bacteria or micro-punctures in the surgeon’s gloves. As a result of the internal investigation, surgeons must now wear thicker gloves or double-up on regular gloves.
But what would repeatedly cause micro-punctures in the surgeon’s gloves in the first place? According to experts, the most likely cause is poor quality surgical instruments.
While few medical professionals were willing to go on record with the BBC, Tom Brophy, a lead technologist with Barts Health NHS (National Health Service) Trust, did. Deeply concerned about what he’s been seeing, he has started collecting evidence showing just how defective some surgical tools are.
Most of these defects cannot be seen with the naked eye, but under magnification, jagged edges and poor quality construction becomes readily evident. Common problems reported by Brophy include:
- Fractured and re-welded instruments, which can harbor and spread bacteria
- Sharp, protruding guide pins on forceps that can lacerate gloves
- Sharp burs and metal fragments that can break off, lacerating gloves and/or pose an infection risk if deposited inside the patient
- Corrosion and pitted metals that can pose an infection risk
- Faulty screw heads
 1 in 5 Surgical Instruments Is Flawed
1 in 5 Surgical Instruments Is Flawed
According to Brophy, 1 in 5 instruments, or about 20 percent of all instruments he receives, are rejected due to flaws that place patients’ health at risk. He even reports receiving used equipment where blood and dried tissue could pose an infection risk.
These tools are somehow recycled and passed off as brand new — something that simply should not occur. Yet it’s happening. Poorly constructed instruments also should not enter the surgical suite, yet they do with frightening frequency. How is all of this possible?
In the U.K., manufacturers and suppliers of surgical instruments must be registered with the Medicines and Health Care Products Regulatory Agency (MHRA), and there are over 900 manufacturers registered.
In December, 2010, following mounting complaints about shoddy quality, the agency issued a warning to all manufacturers saying steps must be implemented to ensure that all instruments are “fit for purpose.”
However, the responsibility for ensuring that quality standards are actually met still rests with the manufacturers, not the MHRA or any separate quality control agency. The suppliers are not even required to inspect the products received from the manufacturer before re-selling them to a hospital.
In all, there are 180 health trusts and boards in the U.K., but Barts is the only health trust that actually employs a technologist to inspect all the instruments before they’re used in surgery.
Disturbingly, when Brophy sent back rejected instruments to an Asian supplier, he was told that the instruments were sent out to another U.K. hospital that accepted them without issue. “Well, of course they’re going to accept them,” Brophy says, “because they haven’t checked them.”
http://articles.mercola.com/sites/articles/archive/2016/12/31/poor-quality-surgical-instruments.aspx
Pro-capitalists say that the current system inspires and forces creativity from people by recognizing a need, and be rewarded financially for the effort. That’s just half of the story, of course.
The question must first be asked, “Was there ever a need for it?”
Was there ever a need for an artificial prosthetic if we can investigate and replicate how a salamander regrow his limb, or tail, in full in just a matter of days?
In short, it’s not just that we have to go past the medical propaganda against alternative protocols, but we also have to deal with the costs of the whole exercise, and the absence of an honest desire to perform those procedures to the best of their abilities and equipment.
Since the profit motive is built into the whole system, we can never see any progress anytime soon. The modern capitalist medical system will continue to find ways to lessen the costs of manufacturing, marketing and installation of these mechanical substitutes to our body parts.
We deserve better than that.
But we can only do it ourselves, or we need to find a selfless medical practitioner who can replicate the procedures of the late Dr. Robert O. Becker.
Or, we can explore a far better system so that the profit motive will be forever done with…
In the meantime, we have to avoid physical trauma, and refrain from unhealthy food as much as possible to be more resistant to infections.
Keep well rested, and do regular brisk walking. Don’t forget to gaze at the sun early in the morning, or late in the afternoon. It’s spiritually refreshing, plus it improves the eyesight!
Happy New Year 2017, everyone!

Good article only it’s not capitalism, it’s Materialism which has separated from Nature.